Ben Johnson, VP, Portfolio & Regulatory, Healthcare, 3D Systems02.05.24
The medical device industry has experienced widespread change in recent years. Advances in data capture and emerging technologies like 3D printing, robotics, and augmented/virtual reality have revolutionized surgical procedures, allowing for more precise and personalized interventions that cater to the unique needs and conditions of individual patients.
Now, patient imaging data segmentation and 3D-modeling design software are integrating deep learning and artificial intelligence (AI) algorithms to expedite the design and development of patient-specific implants and instrumentation. Additionally, advanced preoperative planning portals are aggregating previously siloed processes while improving visualization and communication between surgeons and designers. The ability to automate and streamline personalization workflows can, in turn, help surgeons plan and perform these personalized surgeries in less time. Let’s look at why this is important.
For example, 3D Systems and Enhatch partnered to create VSP Connect, a planning portal that combines AI and semi-automated technologies with FDA-cleared workflows for personalized solutions. It includes advanced segmentation and design software, expert planning services, personalized implant and instrument design, as well as 3D printers and manufacturing processes. The result is a fully integrated experience for surgeons using patient-specific implants and instrumentation with the goal of minimizing procedure times and improving patient outcomes.
By using semi-automated personalization workflows and a centralized portal, healthcare systems can streamline preoperative planning processes and potentially reduce OR time. Expedited planning processes may also positively impact surgical efficacy and outcomes. For example, if surgeons can progress more rapidly from imaging to surgery in oncology cases, they can help mitigate rapid changes within the anatomy and tumors.
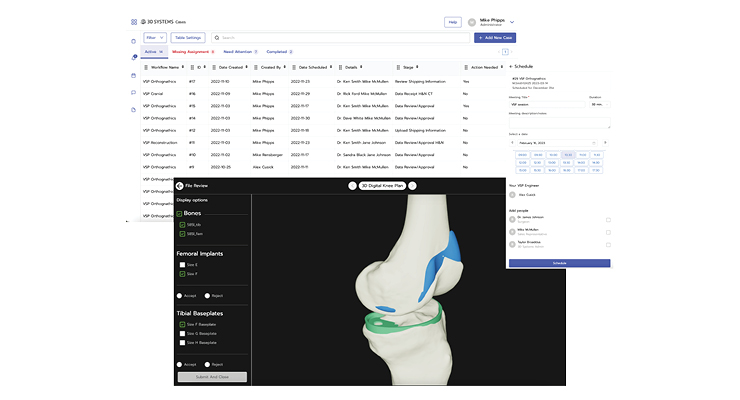
A cloud-based portal offers a centralized workspace for all activities required to plan patient-specific surgical cases. Users can quickly assess where the case is in the preoperative planning process and understand which tasks are required of each team member. Engineers, case planners, surgeons, and medical device representatives can quickly review and engage with each step in the process. If any task requires attention, the portal provides timely alerts to keep the process moving. To help expedite the process for busy surgeons, the portal also allows them to give immediate feedback on surgical plans, resulting in faster reviews and approvals.
Additionally, new capabilities within 3D modeling software enable VR visualization and 360-degree model rotation to evaluate anatomical structures and plan interventions.
Semi-automated workflows and a centralized portal can streamline preoperative planning processes and gain efficiencies that can reduce OR time and increase surgical throughput. Plus, with fewer administrative responsibilities, surgeons are less prone to burnout and can perform surgeries at the scale needed to accommodate the growing demand for orthopedic surgery.
To ensure compliance with regulatory requirements, medical device manufacturers need to collaborate with 3D printing partners that provide compliant technologies and production processes. Moreover, manufacturers should adhere to established protocols that guarantee precision and consistency. Surgical planning teams need to be able to trust that technology is designed to follow a predetermined set of parameters and all portal users work within those parameters.
In addition, the surgical planning team needs assurance all data is protected. Because imaging data is such a crucial part of the process, the technology must comply with HIPAA and GDPR regulations.
According to a survey by the Pew Research Center, 38% of Americans think AI in health and medicine would lead to better overall outcomes for patients.3 AI and deep learning algorithms can help providers expedite responses to interventions, streamline workflows, and allow surgeons to spend less time on lengthy administrative tasks and more time on care for their patients.
References
Benjamin Johnson is vice president of portfolio & regulatory at 3D Systems. His career has spanned more than two decades, focused on the development and commercialization of innovative medical devices. He joined 3D Systems in 2015 through the acquisition of Medical Modeling and has held progressive roles in operations, product development, regulatory, and marketing. Johnson currently serves as a leader in the Healthcare Solutions Group.
Now, patient imaging data segmentation and 3D-modeling design software are integrating deep learning and artificial intelligence (AI) algorithms to expedite the design and development of patient-specific implants and instrumentation. Additionally, advanced preoperative planning portals are aggregating previously siloed processes while improving visualization and communication between surgeons and designers. The ability to automate and streamline personalization workflows can, in turn, help surgeons plan and perform these personalized surgeries in less time. Let’s look at why this is important.
Growing Demand Amid Surgeon Shortages
Whether due to age, overactivity, or obesity putting a strain on bones, the demand for orthopedic surgeries is rising, especially among the elderly. Studies show the number of Americans aged 65 and older will more than double over the next 40 years, reaching 80 million by 2040.1 At the same time, orthopedic surgeons are expected to experience higher rates of burnout as they are asked to do more with less. A recent assessment of the U.S. surgeon workforce in 10 surgical specialties predicts a worsening shortage of orthopedic surgeons, with estimated deficits of >10,000 surgeons by 2030 and 13,000 by 2050.2 This systemic shortage of surgeons reduces providers’ ability to meet patient demand.Improvements Through Automation
As healthcare systems look to mitigate predicted surgeon shortages amid rising surgical demand, patient-specific surgical planning technologies promise to improve efficiencies. Surgeons are choosing to work with device manufacturers that have easy-to-use portals and AI-enabled software that can help streamline the design and delivery of patient-specific medical devices.For example, 3D Systems and Enhatch partnered to create VSP Connect, a planning portal that combines AI and semi-automated technologies with FDA-cleared workflows for personalized solutions. It includes advanced segmentation and design software, expert planning services, personalized implant and instrument design, as well as 3D printers and manufacturing processes. The result is a fully integrated experience for surgeons using patient-specific implants and instrumentation with the goal of minimizing procedure times and improving patient outcomes.
Leveraging Technology to Expedite Interventions
The use of workflow automation in healthcare settings has been increasing in recent years. Automation can help streamline processes, reduce errors, and improve efficiency, which can be especially important in the context of surgery, where precision and coordination are critical.By using semi-automated personalization workflows and a centralized portal, healthcare systems can streamline preoperative planning processes and potentially reduce OR time. Expedited planning processes may also positively impact surgical efficacy and outcomes. For example, if surgeons can progress more rapidly from imaging to surgery in oncology cases, they can help mitigate rapid changes within the anatomy and tumors.
Improving Visualization and Communication
Without integrated workflows, preoperative planning is conducted using multiple disparate applications and tools. Gaining visibility into cases at various stages of planning can be difficult and time-consuming.A cloud-based portal offers a centralized workspace for all activities required to plan patient-specific surgical cases. Users can quickly assess where the case is in the preoperative planning process and understand which tasks are required of each team member. Engineers, case planners, surgeons, and medical device representatives can quickly review and engage with each step in the process. If any task requires attention, the portal provides timely alerts to keep the process moving. To help expedite the process for busy surgeons, the portal also allows them to give immediate feedback on surgical plans, resulting in faster reviews and approvals.
Additionally, new capabilities within 3D modeling software enable VR visualization and 360-degree model rotation to evaluate anatomical structures and plan interventions.
Gaining Greater Efficiency at Scale
With any patient-specific procedure, the process is often managed through multiple, siloed software systems, which can create delays. The slower pace results in longer wait times, delays in scheduled surgeries, and difficulties in accommodating a larger volume of patients. This adds to the complexities of an increasing number of surgeries and the need to alleviate time pressures on surgeons.Semi-automated workflows and a centralized portal can streamline preoperative planning processes and gain efficiencies that can reduce OR time and increase surgical throughput. Plus, with fewer administrative responsibilities, surgeons are less prone to burnout and can perform surgeries at the scale needed to accommodate the growing demand for orthopedic surgery.
Enhancing Compliance with Regulatory Requirements
The U.S. Food and Drug Administration continues to evolve its guidance to ensure quality and efficacy with 3D-printed, personalized medical devices. This is in response to calls for clearer regulation and improved cooperation between manufacturers and regulators.To ensure compliance with regulatory requirements, medical device manufacturers need to collaborate with 3D printing partners that provide compliant technologies and production processes. Moreover, manufacturers should adhere to established protocols that guarantee precision and consistency. Surgical planning teams need to be able to trust that technology is designed to follow a predetermined set of parameters and all portal users work within those parameters.
In addition, the surgical planning team needs assurance all data is protected. Because imaging data is such a crucial part of the process, the technology must comply with HIPAA and GDPR regulations.
Integrating AI: The Future of Patient-Specific Surgery
AI shows great promise in creating efficiencies in the preoperative planning process for patient-specific surgery. Rather than starting from scratch with each design and case, teams can review similar cases to pull suggested models and customize new patient-specific devices. By building on previous successes, teams can process more cases in less time and achieve significant cost efficiencies.According to a survey by the Pew Research Center, 38% of Americans think AI in health and medicine would lead to better overall outcomes for patients.3 AI and deep learning algorithms can help providers expedite responses to interventions, streamline workflows, and allow surgeons to spend less time on lengthy administrative tasks and more time on care for their patients.
References
Benjamin Johnson is vice president of portfolio & regulatory at 3D Systems. His career has spanned more than two decades, focused on the development and commercialization of innovative medical devices. He joined 3D Systems in 2015 through the acquisition of Medical Modeling and has held progressive roles in operations, product development, regulatory, and marketing. Johnson currently serves as a leader in the Healthcare Solutions Group.